Tarsal Coalition
Edited by Peter Stavrou MD
Summary
A tarsal coalition is a condition where one or more of the bones of the hindfoot (talus, calcaneus, and navicular) do not fully separate during development. These bones normally split apart (forming a joint) in the early part of pregnancy when the embryo is developing. The coalition holding the bones together can range from flexible fibrous tissue, cartilage, or a rigid bridge of solid bone. The effect of a tarsal coalition is that the position of the hindfoot tends to be fixed in patients with a tarsal coalition. Sometimes the foot is fixed in a neutral position but sometimes it is fixed in a fairly flatfooted position. In either case, the hindfoot does not move normally.
The most common tarsal coalitions are:
- Talo-calcaneal coalition: In this case the talus (lower bone of the ankle) and the calcaneus (heel bone) have not fully separated.
- Calcaneo-navicular coalition: In this case the front part (beak) of the calcaneus is attached to the outside and lower (lateral) part of the navicular.
- Talo-navicular coalition: This coalition is less common and results when the talar head and the navicular do not fully separate.
Clinical Presentation
Many tarsal coalitions are asymptomatic and people may live their whole life without realizing that they have a tarsal coalition. However, certain tarsal coalitions can create symptoms which in some individuals can be quite significant. The main symptoms are:
- Pain (which can occur in various areas of the foot) and;
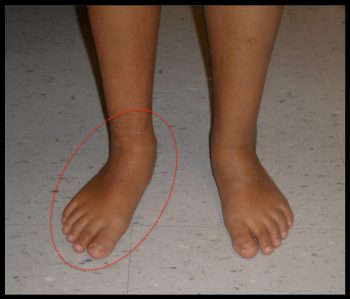
- A fixed foot deformity/stiffness (usually a flatfoot –Figure 1): The most common time that symptoms will occur is during adolescence (ages 12-16). During this time period, children are often growing and gaining weight and therefore more force is going through the foot. At some point the limitations created by the tarsal coalition may lead to symptoms. For example, a fibrous coalition can become irritated creating pain, or a fixed foot position (eg. flatfoot) can lead to an overload of certain tendons (eg. Posterior tibial tendon in the case of a flatfoot) producing tendonitis like symptoms.
- Arthritis. As patients get older they may develop painful arthritis in one or more of their hindfoot joints (eg. Subtalar arthritis or talonavicular arthritis). This occurs because the stiffness of the joints affected by the tarsal coalition leads to increased stress within them that can cause the joint to lose cartilage (arthritis) over time. Patients will often give a story of an injury/sprain that occurred as a teenager that never really got better.
Figure 1: Flatfoot in a Child due to a Tarsal Coalition
Imaging Studies
Often a tarsal coalition can be diagnosed on a plain x-ray of the ankle or the foot. There are certain plain x-ray signs that are classic for certain tarsal coalition including:
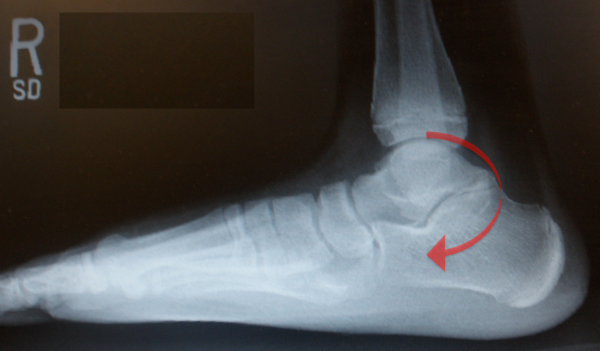
- “C-Sign” (Figure 2): seen in talo-calcaneal coalition – in which the bony contour of the coalition between the talus and the calcaneus form a smooth C-shaped line
- “Ant eater sign” seen in a calcaneo-navicular coalition
Figure 2: C-Sign Demonstrating Talo-Calcaneal Tarsal Coalition on X-Ray
However, in many instances, a tarsal coalition will not be seen on a regular x-ray and a CT scan or MRI will be needed to establish the diagnosis. CT scan can best determine the extent of bone bridging in larger coalitions, but MRI is best for smaller, non-bony coalition lesions.
Treatment
Non-Operative Treatment
A variety of non-operative treatments may be helpful in managing the symptoms of a patient with a symptomatic tarsal coalition. These include:
- Activity Modification: Eliminating precipitating activities (eg. Walking on uneven terrain) or limiting activities in the short-term can be helpful in decreasing symptoms. By decreasing the repetitive load through the painful area symptoms will often settle.
- Comfortable well-fitted shoes: Shoes that help disperse the force evenly up the leg and or limit motion of the hindfoot can help decrease the localized forces going through the hindfoot joint that has the coalition (and the adjacent joints) and thereby decrease symptoms. Typically a shoe with a stiff sole and a slight curve to the sole (rocker-bottom contour) will be more comfortable.
- Orthotics: Inexpensive supportive over-the-counter (OTC) orthotics can help symptoms as well in some cases.
- Ankle Bracing: Ankle bracing such as an ankle lacer or in some cases an Arizona ankle lacer can help limit the motion through the painful areas and can thereby significantly improve symptoms.
- Anti-inflammatory medication: The short-term or regular use of anti-inflammatory medication (provided there are no contra-indications) may be helpful in controlling the symptoms associated with a tarsal coalition.
- Injection: Occasionally a lidocaine (local freezing) will be used to help diagnose the source of pain and a corticosteroid injection may be used to provide some temporary relief of symptoms.
Operative Treatment
In some instances, surgical intervention is warranted. This is the case when symptoms become too severe despite adequate non-surgical management or if either because the symptoms have become too severe or there is a:
- Resection of the Coalition: In certain patients where the coalition is small (e.g. only a part of the joint involved) it may be possible to resect (remove) the fused joint, essentially re-establishing the joint. Coalition resection has a better outcome in younger, skeletally immature patients which often have more flexibility and without permanent damage to the cartilage surfaces of the joint.
- Subtalar Fusion (Arthrodesis): For many talo-calcaneal fusions it may not be possible to save the subtalar joint and surgery to fuse this joint may be necessary.
Fusion is reserved for those joints with extensive coalition (regardless of age), where resection of the coalition would leave an unstable joint, or when the cartilage of the joint is damaged as a consequence of the abnormal stresses placed on the joint by the coalition, such as when a coalition is diagnosed in an adult.
Previously edited by Anthony Van Bergeyk MD
Edited October 31, 2017
mf/ 8.29.19
