Accessory Navicular Bone
(Os Naviculare)
Summary
An accessory navicular bone (also known as an Os Naviculare) is an extra bone on the inside of the foot. It is a common finding on many foot x-rays (5-15%). Most accessory naviculars are asymptomatic (not painful and a normal finding). However, in some patients, the prominent bone on the inside of the foot will create discomfort, which leads to difficulty with shoe fitting. Alternatively, the tissue between the navicular bone and the “extra” accessory part may become irritated and cause discomfort. The diagnosis of a painful accessory navicular is made via physical examination and plain x-rays of the foot. Treatment is usually non-operative, often including a change in shoe wear, activity modification, and sometimes an insole to offload the painful area. However, patients that have ongoing symptoms once non-surgical treatments are tried, may benefit from surgery to remove the prominent accessory navicular and, if necessary, reattach the posterior tibial tendon.
Printable Handout
Clinical Presentation
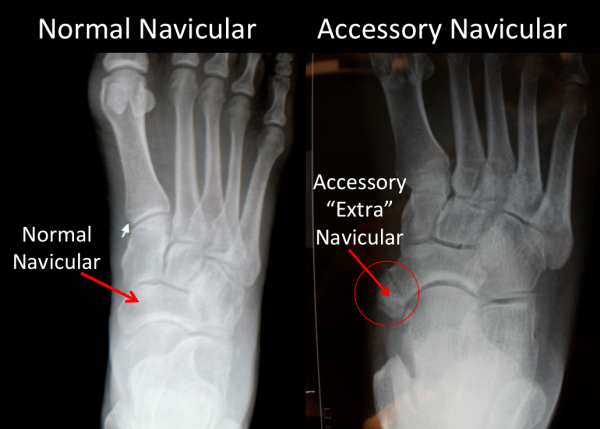
Many people have accessory naviculars (Figure 1) – a prominent extra bone extending from the navicular bone. Depending on the population that is studied between 5-15% of people will have an accessory navicular that is seen on x-ray. Most accessory naviculars are completely asymptomatic. However, some individuals will develop pain on the inside of their midfoot. Pain may occur from the pressure of the shoewear against the prominence, irritating either the bone itself or the fibrous junction where the accessory bone meets the regular navicular. Alternatively, the fibrous tissue or interface connecting the extra-bone with the navicular bone may become painful as a result of tension applied by the posterior tibial tendon through its connection or insertion at that site. Often, individuals will be without symptoms for years, however, a new pair of shoes or a change in their activity level may lead to the onset of symptoms. The accessory navicular itself typically develops during adolescence, when the two areas of the navicular bone fail to fuse together. Upon examining a foot with a symptomatic accessory navicular, there will often be a bony prominence on the inside of the foot, just below and in front of the inside ankle bone (medial malleolus). The size of this prominence will vary from small to quite large. Pressing over this area will often cause discomfort. There may be an associated flat foot deformity as this can occur in patients with an accessory navicular. Stressing the posterior tibial tendon by raising the heel up and down on one foot, or by forcing the foot to the inside against resistance, may aggravate the symptoms as these maneuvers stress the posterior tibial tendon which is attached on the inside of the accessory navicular bone. Patients may walk with a slight limp due to the pain.
Imaging Studies
Plain x-rays are used to determine the size of the accessory navicular. There are three main types of accessory navicular bones:
1) a small bone embedded within the nearby posterior tibial tendon;
2) a triangular shaped bone connected to the navicular by thick cartilage; and
3) a large prominent navicular tuberosity thought to represent an accessory navicular that has fused to the navicular.
If the status of the posterior tibial tendon needs to be assessed or if other problems are suspected, (ex. Navicular stress fracture) it may be necessary to perform an MRI. Although this is not considered routine, an MRI may be helpful in identifying the degree of irritation. An MRI would demonstrate fluid or edema that may accumulate in the bone as a result of the irritation.
Treatment of a Symptomatic Accessory Navicular
Non-Operative Treatment
Many individuals with symptomatic accessory naviculars can be managed successfully without surgery. Standard non-surgical treatment includes:
Appropriate Comfortable Shoes
Shoes that are soft around the inside of the ankle can allow for any excess prominence of bone. Therefore, it is recommended that either shoes with plenty of padding and space in the ankle area are purchased, or pre-owned shoes can be modified by a shoemaker to create extra space in this area. For example, many patients will get their ski boots expanded in the area around the prominence, minimizing irritation. In addition, a shoe with a stiff sole will help disperse force away from the arch of the foot during walking, thereby minimizing the force on the posterior tibial tendon. An arch support may help decrease the stress applied by the posterior tibial tendon. If necessary, an ankle brace applied to provide more substantial support to the arch may be successful where a simple arch support fails.
Application of local padding
Often applying local foam or gel padding can help improve symptoms. Both can be purchased at many pharmacies.
Activity Modification
If symptoms have been aggravated by an increase in activity level, backing off on activities in the short term can be helpful. The foot is subject to a lot of repetitive loading during walking, and therefore minimizing this force will often help symptoms to settle. After symptoms have settled, the activity level can then be gradually increased.
Weight Loss
Excess weight will increase the force on the posterior tibial tendon as it inserts into the accessory navicular and will tend to precipitate or aggravate symptoms. If a patient with a symptomatic accessory navicular is overweight, then losing weight can be very helpful. Even losing 5-10lbs will decrease the amount of force going through the foot with each step by as much as 15-30lbs. This is because the foot acts like a lever serving to magnify the force absorbed by the foot with each step.
Operative Treatment of a Symptomatic Accessory Navicular
If non-operative treatment fails to relieve the patient’s symptoms, surgical intervention may be warranted. The standard operative treatment of an accessory navicular is a Kidner procedure. However, if surgery is undertaken it is important that it addresses the underlying source of the patient’s pain. Surgical treatment may include:
Modified Kidner Procedure (Resection of the Prominent Accessory Navicular)
The Kidner procedure involves resecting the prominent accessory navicular and ensuring that the posterior tibial tendon is still attached to the bone and able to function well. Often the prominent bone can simply be shelled out from its position relative to the posterior tibial tendon, which leaves the tendon intact. However, if the tendon is loose and floppy once the extra bone has been removed, suturing or together is required as a means of attaching it into the remaining navicular bone.
Kidner Procedure
In the original Kidner procedure, the entire posterior tibial tendon was released from the navicular and then rerouted through a drill hole placed through the navicular. The original Kidner procedure is now rarely used as a means of treating an isolated accessory navicular. Instead, a modification of the Kidner procedure has become more commonplace. The modified Kidner procedure consists of carefully removing the accessory and anchoring the posterior tibial tendon to the surface of the navicular where the accessory was removed. The repair may be done by passing a suture through the tendon and then through drill holes in the navicular, or by using a suture anchor.
Fusion of the Accessory Navicular to the Navicular
Fusion of the accessory navicular to the navicular with screws is required when there is a large accessory navicular bone and removal of this bone would reduce the articular surface of the Navicular to the talus (coxa pedis). Fusion will relieve pain without disrupting the tibialis posterior tendon insertion nor narrowing talar head support.
Recovery
In most instances, a patient’s recovery will be as follows:
- 0-6 weeks: Immobilization (in cast or cast boot) non-weight-bearing or touch weight-bearing
- 6-10 weeks: Increasing activity in a cast boot. Physical therapy to work on strength and balance
- Full recovery can take many months.
In some patients (where the posterior tibial tendon is still intact and functioning) the treating surgeon may allow weight-bearing as tolerated in a cast boot immediately after surgery.
Printable Handout
Edited on September 19th, 2023
(Previously edited by David Townshend FRCS, Gwyneth deVries, MD, FRCSC, Jean Brilhault, MD, Michael Castro, DO)
sp/9.19.23